According to the World Health Organization (2023), an estimated 180,000 deaths every year globally are caused by burns, with the vast majority occurring in low- and middle-income countries, with non-fatal burn injuries being a leading cause of morbidity. In Vietnam, it is estimated that 80,000–100,000 people suffer from burn injuries per year (Lam et al, 2021). In a study to determine the characteristics of treatment results and mortality risk factors of burn patients over a 10-year period (2010–2019) conducted in a national burn centre in Hanoi, it was reported that the length of hospital stay is 16.84 ± 14.61 days, with a mortality rate of 3.4% (Ngo et al, 2020).
Burns have been described as under-appreciated injuries (Jeschke et al, 2020). These injuries are accompanied by an immune and inflammatory response, metabolic changes and distributive shock that can be challenging to manage and can lead to multiple organ failure (Jeschke et al, 2020).
Management of a patient with a severe burn injury includes respiratory support and management, treatment of inhalation injury (if present), fluid resuscitation, cardiovascular stabilisation, pain control and management of the burn wound (Vivó et al, 2016).
The objective of burn management is to stop the burning process, minimise scarring, relieve pain, prevent infection and prevent future complications, such as dysfunction of the injured site or burn shock (Kim et al, 2022). However, infection, pain, and hypertrophic scarring remain major challenges in burn management (Wang et al, 2017).
Wound management in burns
Wound infection is the most serious complication of burns in the acute phase following burn injury. Approximately 73–85% of all deaths that occur within the first 5 days of injury are due to sepsis (Kim et al, 2022).
Wound dressings utilised in burns can protect from infection and further skin damage, promote re-epithelialisation, and decrease pain (Liu et al, 2017). Topical antimicrobials are indicated when there is clinical suspicion of risk of infection, or when wound infection is evident (Cartotto, 2017).
Silver sulfadiazine, a topical silver sulphonamide antibacterial agent, has been widely used for burn wound treatment since the 1960s, even though evidence to support its effectiveness in promoting wound healing is lacking (Rosen et al, 2015; Nimia et al, 2019; Vishwanath et al, 2022). Its negative impact on the wound healing process has been documented , including altered activation of macrophages and cytotoxicity on keratinocytes and fibroblasts (Punjataewakupt et al, 2019; Abul Barkat et al, 2023).
Topical cream is also known to form a pseudo-eschar that is loose at the edges, which could promote bacterial proliferation (Tenehaus and Rennekampff, 2018).
When considering wound antiseptics, it is recommended to select agents that act immediately, have broad-spectrum and long-lasting activity against microorganisms, but also have a safe activity on both healthy and injured skin, providing good tolerance without adverse effects (International Wound Infection Institute [IWII], 2022).
Polyabsorbent fibre pad dressing with technology-lipido colloid and silver (TLC-Ag)
Polyabsorbent fibres (Magnet Fibres™, Laboratoires Urgo, France) are designed to continuously debride slough due to the bonding of the negatively charged fibres and positively charged regions in slough, trapping bacteria and other non-adherent or devitalised material in the dressing, which is then removed when it is changed (IWII, 2022; Mayer et al, 2024; Nair et al, 2024).
The polyabsorbent fibres are available as a pad impregnated with a lipido-colloid and silver sulphate healing matrix (TLC-Ag healing matrix, UrgoClean Ag®; Laboratoires Urgo, France). This dressing was evaluated in a clinical trial in patients with venous leg ulcers (Dalac et al, 2016). At the final visit, r52.1% of wounds were debrided, with a relative slough reduction of 62.5% (median) while the clinical score (maximum value of 5, based on inflammatory clinical signs) decreased from 4.0 to 2.0.
In a real-life observational study, the dressing was used in 2,270 patients with various aetiologies, including 134 patients with burn injuries (Dissemond et al, 2020). Clinical improvement in wound healing was reported in 98.9% of acute wounds, with a wound closure rate of 68.5%, and the dressing was well tolerated and well accepted by both patients and health professionals.
In another study of 14 patients from the UK with deep sloughy burns treated with the TLC-Ag polyabsorbent fibre pad dressing, debridement was usually fully achieved by the third or fourth application (Edwards and Karuppan, 2017). All wounds showed a marked improvement, and bioburden control was achieved with no further signs of infection, while the dressing was easy and painless to apply and remove.
The cases
The authors encounter patients with burn injuries of various severities every day in their practices, in their respective burn centres. They have evidence-based protocols and standards of holistic care in place, but are always interested to evaluate new evidence-based dressings in the local treatment of the patients’ wounds. Although the majority of clinical evidence for the TLC-Ag fibre pad dressing is from treating chronic wounds, it was of particular interest to note the cases in burn patients involved in the German observational study (Dissemond et al, 2020), and the cohort from the UK (Edwards and Karuppan, 2017).
Case 1 (Le Phat Dat, MD)
A 62-year-old woman with history of well-controlled hypertension, sustained a scald injury to the upper one-third of her inner thigh, lower abdomen and groin, with a total estimated at 6% total body surface area (TBSA). The wound was being managed with saline and povidone iodine gauze dressings but was referred to the burn centre after 15 days because the wound on the left thigh was covered by tenacious slough, with profuse swelling in the region with signs and symptoms of local infection [Figure 1A]. The wound was cleansed with normal saline and chlorhexidine 0.05%, with the TLC-Ag polyabsorbent fibre pad dressing as the primary dressing, held in situ with sterile gauze. Dressing changes were conducted on alternate days. Antibiotics were administered throughout the treatment.
Within 4 days, the sloughy tissue had reduced (from ~80% to ~30%) [Figure 1B]. Within 12 days, the wound bed was almost entirely clean and free of slough [Figure 1C] and the patient was discharged. She was managed by home care service with a lipido-colloid healing matrix contact dressing (UrgoTul, TLC, Laboratoires Urgo, France). The wound continued to progress [Figure 1D] and was healed after approximately 3 weeks.
Case 2 (Le Phat Dat, MD)
A 34-year-old woman, with no known medical history, sustained a burn with petrol on her right thigh. The wound was managed with normal saline and chlorhexidine 0.05% cleansing, silver sulfadiazine cream and cotton gauze. The patient was referred to the centre 8 days after the injury, as the wound was not progressing due to local infection, suspected biofilm presence and lack of proper debridement [Figure 2A].
The wound was cleansed with saline and chlorhexidine 0.05% and the TLC-Ag polyabsorbent fibre pad dressing was applied, with sterile gauze as the secondary layer. The dressing was changed on alternate days. Antibiotics were prescribed during the course of the treatment.
Within 8 days, the wound was looking healthier [Figure 2B], and a skin graft was applied. The patient was discharged thereafter.
Case 3 (Le Van Loc, MD)
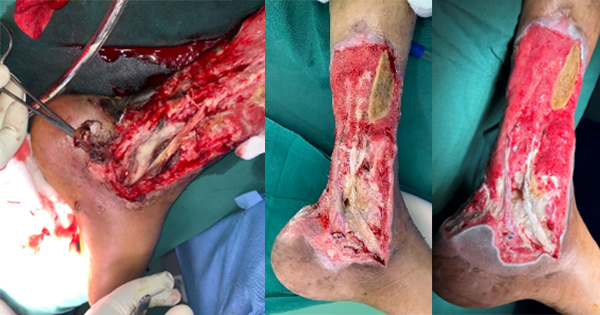
A 45-year-old man sustained a 39% TBSA oil flame burn (mostly on his back) at his place of work on an oil rig. The patient was referred immediately after the incident. Surgical debridement was performed, and the wound area was cleansed with normal saline, povidone-iodine and chlorhexidine 0.05% [Figure 3A]. The TLC-Ag polyabsorbent fibre pad dressing was applied as the primary dressing with sterile gauze as the secondary layer. The dressing was changed on alternate days. Blood products (due to patient’s anaemia), albumin, antibiotics, analgesics, and nutrition and vitamin supplements were prescribed.
Within 5 days, the wound appeared healthier, with substantial reduction in burned area, exudate levels, and pain. The wound bed also looked healthier [Figure 3B]. Further progress was noticeable at subsequent reviews [Figures 3C and 3D]. After 2 weeks of treatment with the TLC-Ag polyabsorbent fibre pad dressing, the wound bed appeared healthy, with the presence of granulation tissue and epithelialisation [Figure 3E]. Thereafter, the neutral TLC healing matrix contact layer was used, as there was no further need for debridement. The dressing was changed every 3 days until hospital discharge (10 days with the neutral TLC).
Case 4 (Le Van Loc, MD)
49-year-old male with no previous medical history, sustained an occupational accident, resulting in deep partial-thickness second-degree steam burns to the neck, trunk, and scattered areas on all four extremities (32% TBSA) and was referred to the clinic immediately. The wound area was cleansed with normal saline, povidone-iodine and chlorhexidine 0.05% [Figure 4A]. The TLC-Ag polyabsorbent fibre pad dressing was applied as the primary dressing, with sterile gauze as the secondary layer. The dressing was changed on alternate days. Antibiotics, analgesics, and nutrition and vitamin supplements were prescribed.
Within 4 days, the wound bed demonstrated a marked reduction of slough [Figure 4B], with the wound almost completely healed within 2 weeks [Figure 4C]. The patient was discharged with complete healing after 20 days.
Case 5 (Le Van Loc, MD)
A 55-year-old man with no previous medical history, sustained a gasoline-related flame burn during his work as a motorcycle mechanic. After the injury, the wound was cleansed with normal saline, povidone-iodine and chlorhexidine 0.05% and a silver sulphadiazine cream was applied. One day post injury, the patient was referred for further management. The wound was mostly covered with wet slough, with maceration present on the palm of the hand [Figure 5A]. The same cleansing method was applied, and the TLC-Ag polyabsorbent fibre pad dressing was applied as the primary dressing with sterile gauze as the secondary layer. The dressing was changed on alternate days. Antibiotics, analgesics, and nutrition and vitamin supplements were prescribed.
Within 12 days, the wound bed was almost completely covered with healthy tissue [Figure 5B] and, within another 5 days, the wound was healthy and clean enough to change the primary dressing to the TLC healing matrix contact layer [Figure 5C]. The patient was discharged 20 days post-injury, with a healed wound.
Case 6 (Hoang Van Vu, MD)
A 25-month-old boy accidentally pulled a kettle of boiling water from a table, resulting in a scald injury. Initial first aid with cool water irrigation was administered, and the child was transferred to a provincial hospital for emergency management, including IV fluid resuscitation, analgesia, and initial wound dressing comprising of povidone-iodine and saline cleansing and sterile gauze. Within 11 hours of the injury, he was referred to the Vietnam National Burn Hospital and was admitted to the intensive care unit (ICU) in a state of profound burn shock, requiring aggressive resuscitation. The burn injuries were extensive, involving approximately 40% of the TBSA. The maximum depth of the wounds was 5mm, with some small areas identified as third-degree burns. The anterior thorax and abdomen showed ruptured bullae with denuded skin, exposing a hyperaemic wound bed covered with extensive pseudo-membranes [Figure 6A]. The wounds were again cleansed with normal saline and the TLC-Ag polyabsorbent fibre pad dressing applied as the primary dressing with a secondary layer of sterile gauze with daily dressing changes. Antihistamines and antibiotics were also prescribed. Within 12 days, healthy tissue and epithelialisation was evident over 95% of the wound [Figure 6B]. The dressing changes were reduced to alternate days. After three days, parts of the wound were grafted successfully [Figure 6C].
Case 7 (Hoang Van Vu, MD)
A 38-year-old man sustained severe thermal injuries following an occupational accident with molten metal that ignited his clothing, resulting in extensive flame burns. The patient was initially transported by co-workers to the Provincial General Hospital, where he received emergency management, including intravenous fluid resuscitation, analgesia and wound cleansing. He was subsequently transferred to the Vietnam National Burn Hospital and admitted to the ICU in a state of profound burn shock, necessitating aggressive haemodynamic resuscitation. On examination, the patient presented with extensive deep burns covering approximately 60% of the TBSA. The posterior torso exhibited ruptured bullae with areas of skin denudation, revealing a hyperaemic wound bed overlaid with widespread pseudomembranous slough [Figure 7A]. The wound was cleansed with normal saline and the TLC-Ag polyabsorbent fibre pad dressing was applied as the primary dressing with a secondary layer of sterile gauze. Daily dressing changes were performed for 8 days and alternate days thereafter. By 14 days post-injury, progress was noted, with substantial reduction in wound area and the achievement of a healthier wound bed [Figure 7B]. Further progress was recorded after 22 days of treatment [Figure 7C], and 28 days [Figure 7D]. When the wound was nearly healed, the patient was transferred to the Department of Physical Therapy and Rehabilitation for continued care and was discharged about one week later, with complete wound healing.
Case 8 (Nguyen Phuc Hiep, MD)
A 72-year-old man was admitted to hospital with second-degree burns caused by ethanol ignition. The burn covered 5% of the TBSA, involving the neck, anterior chest, right shoulder, and back. The wound had been treated previously for 7 days with normal saline, povidone-iodine and sterile gauze. On referral [Figure 8A], the wound was cleansed with normal saline and the TLC-Ag polyabsorbent fibre pad was applied as the primary dressing with a secondary layer of sterile gauze, with daily changes. After 9 days of treatment, the wound area was reduced, with a visibly healthier wound bed and, after 11 days, the primary dressing was changed to the TLC healing matrix contact layer until complete healing.
Discussion
Burns are unfortunately common injuries, and their treatment remains challenging and complex, necessitating effective local treatment that facilitates healing. Burn wound treatment targets should focus on prevention of infection and removal of dead tissue, while minimising scarring and restoring function (Siu et al, 2025). The rationale for using antimicrobial dressings is to reduce microbial pathogens that delay wound healing, by producing inflammatory mediators and metabolic toxins (Rogers and Jeschke, 2016). The current understanding is that superficial or superficial partial-thickness burns will heal with the appropriate topical treatment (Neelon et al, 2025).
The clinical evidence behind the TLC-Ag polyabsorbent fibre pad dressing includes both a non-comparative clinical trial, as well as a large observational study and case series (Dalac et al, 2016; Dissemond et al, 2020) with specific evidence and positive outcomes in more than 150 patients.
The clinicians wanted to further evaluate the dressing in their own clinical practices in Vietnam. The eight cases presented provide a range of burns in patients aged 2–72 years, with different causal agents, locations, severities, depth and surface areas. All wounds were resolved in a relatively short period (ranging from 8 to 17 days of treatment), with good aesthetic results at the end of the wound healing process.
Conclusion
Although this may be a small cohort of patients, the results achieved are encouraging and aligned with results shown in previous publications. This outcome has prompted the clinicians to adopt the TLC-Ag polyabsorbent fibre pad dressing as part of their holistic standard of care in the management of similar burn patients.