The Covid-19 pandemic led to mandated social distancing and self-isolation in order to prevent spread of infection (Yuki et al, 2020). As a result, the incidence of symptoms of fear, depression and anxiety significantly increased, with mental health sufferers being more at risk of exacerbation of their symptoms (Yao et al, 2020). Many outpatient activities and home visits were cancelled or postponed due to infection risk and staff redeployment.
This case report discusses a patient with pre-existing mental health issues, who was being treated with compression garments for chronic lower limb lymphoedema secondary to lumbosacral myelomeningocele (spina bifida). Due to enforced social isolation, combined with deteriorating mental health, the patient was found in a state of neglect with his self-applied compression stockings rolled down to his ankles, causing a tourniquet effect and leading to bilateral lower limb ischaemia. This ultimately necessitated amputation of his left foot.
This case highlights the negative effect of Covid-19 on vulnerable patients, particularly those who live alone, and suggests that patients’ mental and social state should be considered and monitored when prescribing compression garments. To our knowledge there are no previous reports of this nature, nor guidance on the use of compression therapy in patients with unstable mental health.
Case report
A previously independent 53-year-old man, with a history of spina bifida, with related neurogenic bladder, hydrocephalus, hypertension and chronic lymphoedema secondary to lumbosacral myelomeningocele (spina bifida), was admitted to hospital in a state of severe neglect in January 2021.
The patient had first presented to his GP in 2018 with bilateral leg swelling after being admitted to hospital via the emergency department due to a fall, where he was found on admission to have oedematous legs, superficial ulcers and socks that were causing a tourniquet effect on his feet. However he failed to attend the majority of surgeon-led lymphoedema clinic appointments offered to him, and cancelled nurse led appointments at short notice. He was prescribed Jobst farrow wrap lite below knee leg pieces, size medium/regular, with a pressure of 20–30mmHg, which he self-applied, found helpful, and after commencing a regular exercise bike routine, was discharged. The patient’s father was also present at the GP consultation and noted his son had heightened symptoms of depression, with a strong reluctance to care for himself. In 2019, the patient was prescribed fluoxetine, a selective serotonin reuptake inhibitor, to help with these symptoms.
By 2020, he was receiving regular district nurse and lymphoedema specialist nurse home visits to fit below-knee and foot Haddenham Easywrap Strong Leg compression wraps (Haddenham Healthcare, Long Crendon, Buckinghamshire, UK), as his skin care was now poor, the skin was weeping, and he had developed further dependent oedema due to sleeping in his chair.
The pressure requirements of these wraps were now 30–40mmHg, and the sizes of the wraps were reduced over a 6-month course of visits from XL to regular bilaterally, indicating adherence with his garment protocol. He had again taken up cycling and the lymphoedema symptoms improved. During a home visit in August 2020, it was noted that the swelling had reduced significantly; his skin was intact, hydrated and pliable; mobility had improved and he could now fit his own shoes. Therefore, it was decided that he no longer needed nurse-applied compression wraps and would be more suited to self-applied flat knit stockings instead. He was prescribed Jobst Elvarex knee class 2 closed-toe stockings bilaterally as well as Epimax to manage his own skin care.
A 3-month follow up was organised to assess his progress; however, due to Covid-19 and other unforeseen circumstances, this appointment did not transpire. By this time, the patient had been avoiding going outside for fear of the pandemic, restricting his interaction with his family, and denying them access to his home.
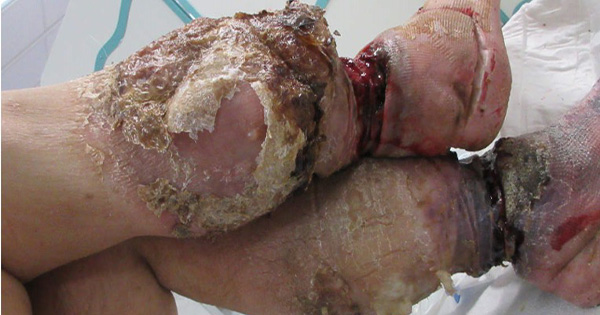
In January 2021, a month after his proposed follow-up by district nurses, he was found in a state of severe neglect, with the self-applied compression garments rolled down to his ankles. These were causing a tourniquet effect, leading to significant ulceration of the ankles and compromised vascularity of the feet (Figures 1 and 2). He also had a sacral pressure sore.
He was critically unwell, requiring immediate resuscitation and dialysis due to severe acute renal failure, and subsequently underwent a left above knee amputation due to a non-viable left foot (Figure 3). The right foot retained vascularity and this continued to improve throughout his admission. He was profoundly anaemic (Hb 54g/1; normal range is 130–180g/1), requiring transfusion.
Psychiatric review on admission confirmed he was acutely paranoid and experiencing suicidal ideation and olfactory hallucinations. He was diagnosed with delirium on a background of suspected depression and a suspicion of schizophrenia which had been originally queried in 2017 by the GP; however, this had not been formally pursued or diagnosed at that time.
Over the following weeks of admission, he became non-verbal with flattened affect (lack of expression of emotion), and was treated for hypoactive delirium. It was decided he would require full-time care on discharge. After the leg amputation, the patient continued to decline mentally and refused to eat. During his admission he contracted and recovered from Covid-19. He died 3 months after admission from multi-organ failure secondary to proteus mirabilis sepsis, and an incidental Covid positivity.
Discussion
Lymphoedema is a progressive, chronic and debilitating disease characterised by tissue swelling caused by the build-up of interstitial fluid arising from impaired lymphatic vessels (Rockson, 2001). The chronic accumulation of protein-rich fluid within the adipose tissue and interstitium exceeds the capacity of the lymphatic system. Swelling can occur anywhere in the body, including the extremities, abdomen, trunk, head/neck and genitals. Lymphoedema is classified as either primary or secondary (Sleigh and Manna, 2020). Primary lymphoedema is an inherited condition that results in the malformation of lymphatic vessels, affecting 1 in 100,000 people worldwide (Smeltzer et al, 1985). Secondary lymphoedema results from injury or obstruction of the lymphatic vessels, and is more common (Greene, 2015). In the developed world, the majority of lymphoedema cases are due to either cancer or the treatment of malignant lesions, including local radiation therapy, medical therapy and surgical removal of lymph nodes (Lyons and Modarai, 2019).
Lymphoedema management can be considered in three stages: “primary” prevention and risk reduction prior to lymphoedema onset; “secondary” prevention for treating early stage lymphoedema, and “tertiary” prevention for treating late stage lymphoedema. Decongestive lymphatic therapy (DLT) in the form of manual lymphatic drainage, exercise and compression garments, together with education for skin care can be used to help alleviate symptoms, but are not in themselves a cure (Executive Committee of the International Society of Lymphology, 2020).
Compression bandages (acting as both secondary and tertiary preventive techniques) aim to move excess fluid out of the affected limb and minimise the effect of further fluid build-up. Routine skin care has been shown to keep the underlying skin in good health and reduce the patient’s risk of developing cellulitis and other infections which would put further strain on the lymphatic system and propagate swelling (Nowicki and Siviour, 2013). Regular exercise of the affected limb aids lymphatic drainage. However, the effect of specialised massage techniques is still debated (Müller at al, 2018).
In a smaller number of cases, surgery can be used, such as liposuction, removal of excess skin and underlying tissue, or the restoration of the lymphatic system via lymphovascular anastomosis (Granzow, 2018).
Quantitative studies have shown that the incidence of depression and anxiety is higher in patients with lymphoedema than the general population (Morgan et al, 2005; Monteiro et al, 2023). Chronic and disabling conditions are risk factors for depressive episodes, while a Danish study of melanoma-related lymphoedema patients found that health-related quality of life scores were significantly worse than non-lymphoedema melanoma patients, particularly in relation to social functioning, fatigue, pain and body image (Gjorup et al, 2017).
This patient was showing excellent progress with his lymphoedema management, with a reduction in the size of garments provided and a subsequent change from nurse-applied to self-applied stockings. He was adherent to his treatment and had increased his exercise routine to further improve his symptoms, indicating good self-care and positive outlook.
Sadly, there was a clear decline evident in his mental health around the autumn of 2020, which correlated with his withdrawal from lymphoedema services. He admitted to being fearful of contracting Covid and chose to avoid social interaction, even with family and friends.
The harmful psychiatric effects of social isolation have been frequently noted, especially in those with pre-existing medical conditions (Teuton 2018; Public Health England 2020, O’Connor et al, 2021).
In Scotland, one-third of the population lives alone, with 40% of this group of pensionable age, a group particularly at risk of isolation during a period of social distancing (Scottish Government, 2018). Similarly, risk factors for neglect include depression, old age, dementia, poor reasoning/memory, untreated mental health problems, longstanding and untreated disease, poor diet and alcohol/substance misuse.
This patient possessed several of these risk factors, indicating he was highly vulnerable to self neglect going into the pandemic. Aside from his chronic lymphoedema and likely undiagnosed depression, he lived alone, had missed hospital appointments and, most importantly, had a recent history of a similar tourniquet effect of his rolled-down socks during a previous admission in 2018, indicating prior self-neglect. These factors could have prompted closer monitoring of his physical and mental wellbeing within the community.
Conclusion
There is no guidance available in the literature on the use of compression garments in patients with mental health issues. This case highlights an extreme sequela of Covid-19 on a previously adherent lymphoedema patient with underlying mental health issues.
Depression or unstable mental health conditions which can result in neglect could be seen as a contraindication to compression garments as even “low” pressure garments, as in this case, can cause significant injury if not used appropriately or with timely and appropriate therapist/clinical support.
We suggest patients having compression garments should be reassessed on a regular basis in terms of their overall physical and mental health to ensure appropriate use of compression garments.
Consent
Consent to publish was provided by the patient.