Skin flap necrosis can be devastating for the microsurgeon after long hours of effort and meticulous surgical techniques. Although many extrinsic and intrinsic factors have been discussed in the literature, it is still difficult to ascertain the precise cause of a flap failure other than insufficient arterial blood supply (Kerrigan, 1983).
Free superficial circumflex iliac artery perforator (SCIP) flap has been described as a versatile reconstructive option (Koshima et al, 2004; Yoshimatsu et al, 2021).
The usage of vascularised lymph node transfers a treatment option for lymphoedema has been reported to have a high success rate in both lymphoedema and tumour surgery (Mardonado et al, 2017; Yoshimatsu et al, 2021).
Flap necrosis is caused by insufficient blood supply, leading to a decreased supply of oxygen and nutrients to the flap. There are many possible causes, including venous thrombosis, infection, arterial thrombosis and haematoma (Culliford et al, 2007). One of the most common intraoperative findings during a flap exploration is an atherosclerotic, damaged or inappropriate vessel (Suominen and Asko‐Seljavaara, 1995).
Steal syndrome is a phenomenon whereby blood is diverted away from one region of circulation to another, causing a deficiency in the blood supply to the original region.
Here, we share our experience of a lymphoedema surgery using SCIP flap with an unfavourable outcome of flap necrosis. There were multiple contributing factors, but we focus on steal phenomenon initiated by nitrates and the undetected preoperative total occlusion of the tibial posterior artery that may have led to this poor outcome.
In this case, we believe that steal syndrome occurred when nitrates were used, in such way that the blood supply shifted from the flap into the peripheral circulation that was already reduced due to occlusion caused by old atherosclerosis. This resulted in reduced blood supply to the flap and contributed to the flap necrosis.
Case report
An 80-year-old man presented with a known case of stage 2–3 lymphoedema of 3 years’ duration in the right leg. He had prostate cancer, arterial hypertension and had undergone surgery for prostate cancer together with inguinal lymph node dissection 5 years prior to the lymphoedema onset. He has undergone lymphatics-venous anastomosis (LVA) twice, which improved his thigh circumference but not his lower-leg swelling. His other comorbidities included non-ST-elevation myocardial infarction more than 10 years earlier and type 2 diabetes, both of which were only revealed by the patient after his operation.
Lower limb clinical and Doppler assessment showed good pulsation of distal arteries despite preoperative ankle brachial index being borderline. An Doppler of bilateral lower-limb venous status showed no deep vein thrombosis or venous insufficiency. He was cleared by the cardiologist and anaesthetist before his operation. Surgery was subsequently planned for simultaneous lymphatics — venous anastomosis and free SCIP flap surgery.
A two-team approach was undertaken during the operation. While the SCIP flap was being harvested from the donor site by one team, simultaneous LVAs and preparation of the blood vessel at the recipient site were performed by another team. The duration of the operation was 9 hours.
During the operation, we found that the arterial blood vessel at the recipient site was atherosclerotic (Figure 1). Two end-to-end arterial anastomosis with a vessel diameter of 1 mm were attempted before a third successful anastomosis proximally to the atherosclerotic vessel. Vein anastomosis was uneventful.
Postoperative flap monitoring was done in intensive care unit using ultrasound Doppler and clinically (Figure 2). On day 3 after the surgery, the patient had an episode of significant hypertension, with systolic blood pressure of 200 mmHg and diastolic of 90 mmHg. He was treated with a stat dose of 0.4 mg nitroglycerin and was stabilised.
After about 10 hours, there was no Doppler signal detected on the flap. Clinically, the flap had no sign of recapillarisation, but remained warm with good turgor. Flap exploration was arranged immediately and arterial thrombosis was found to be the cause of the compromised blood flow into the flap.
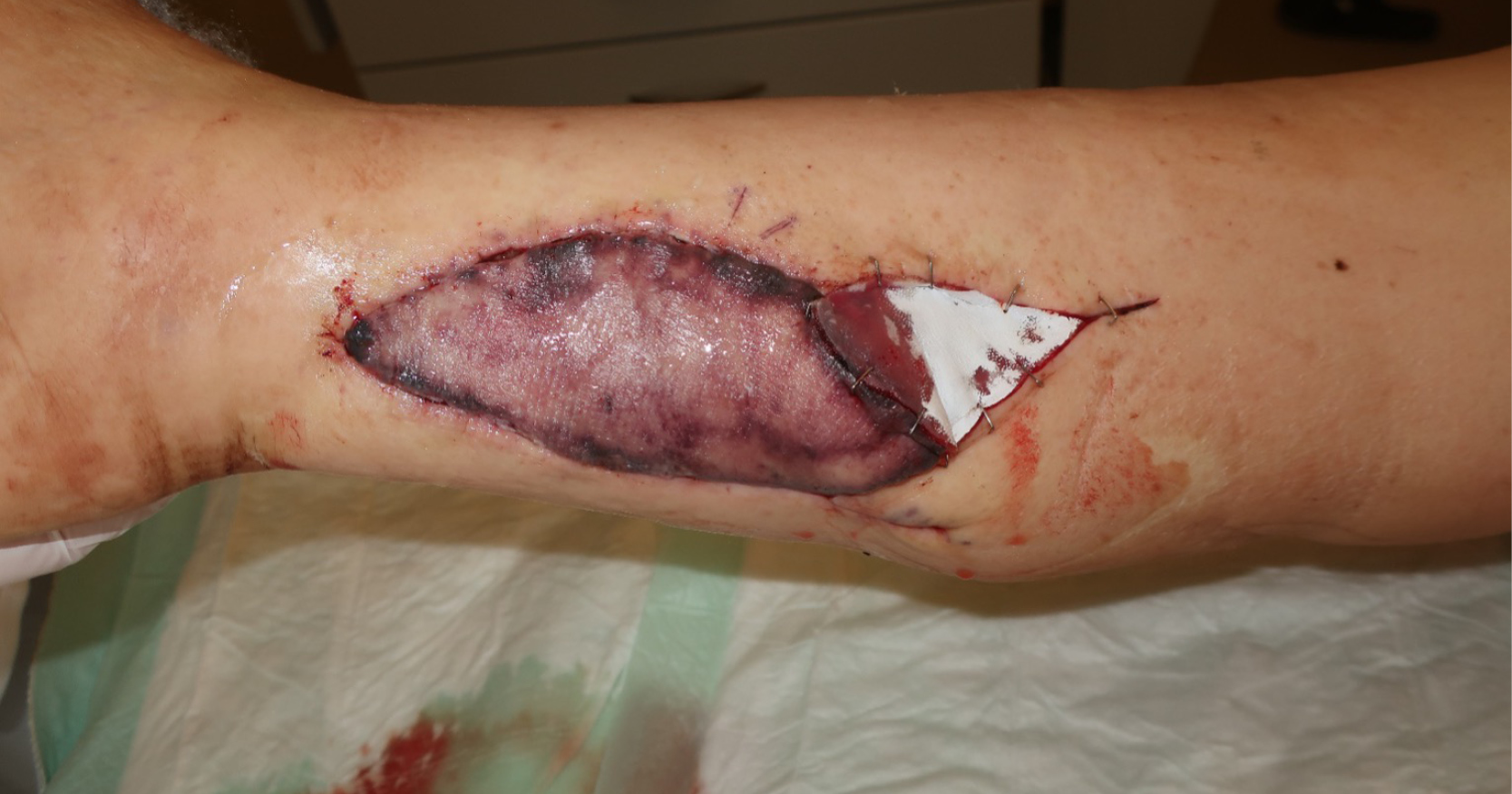
Two subsequent revisions followed, with each new anastomosis being more proximal than the previous one. At the last revision, we found an old, totally occluded, tibial posterior artery, around 7 cm distal to its origin from popliteal artery (Figure 3). Ten hours after the final revision and IV prostaglandin administration, the patient had a myocardial infarction (MI), which also compromised the flap, and the flap was not explored further (Figure 4). Two weeks later, we undertook a total flap debridement and the wound was covered with a split skin graft.
Overall, the patient’s leg circumference markedly reduced 1 day after the first operation. The patient was discharged and follow-up showed a well-healed wound. At follow-up, his lymphoedema leg was markedly softer; however the circumference measures showed little change (Table 1).
Discussion
In general, free flap use in lower limbs has been reported to have a successful rate with approximately an 8% rate of flap failure (Culliford et al, 2007). In a lower limb with peripheral vascular disease, early flap revision rates as high as 16% have been described (Randon et al, 2009).
In our patient, we found that the recipient vessel was atherosclerotic, and all three flap explorations were caused by arterial thrombosis. A flap thrombi usually occurs within the first 2–3 days after surgery (Kroll et al, 1996; Chen et al, 2007). In our case, the flap was first detected to be compromised on day 3–4 after surgery.
In retrospect, in our case, although clinically distal pulses were palpable and detectable with Doppler, the donor vessels to the flap were fed by collateral vesselss only. Our patient had a severe atherosclerotic arterial wall, and arterial flow was suboptimal during the initial operation. It was not the normal pulsation as we expected from a healthy tibial posterior artery. With each re-anastomosis being more proximal than before, arterial flow during the revisions decreased for the flap perfusion, coming closer to the total occlusion of tibial posterior artery resulting to the decreased of collateral inputs as well. During the third revision, total arterial occlusion due to a scarred vessel (Figure 3) was found. Therefore, the segment was resected, and the anastomosis was created proximal to it, with a very good flow after anastomosis. We also used IV heparin perioperatively throughout all revisions.
In hindsight when examining the case and with the knowledge of old arterial total occlusion due to underlying atherosclerosis of the peripheral lower limb vessels, we hypothesised that haemodynamic supply to the flap was initially by collateral vessels. When nitroglycerin was administered for the high blood pressure, a steal syndrome occurred in the free flap, resulting in slower blood flow and then thrombosis of the flap.
Even after two successful revisions, the collaterals became less and less effective by shortening the tibial posterior artery more proximally with each revision and becoming closer to the total occlusion site. With inadequate flow in the collateral vessels, the time between thrombosis and progression of flap to its demise became quicker.
At the third revision, an old total occlusion was found and the anastomosis proximal to this occlusion showed the best flow among all anastomosis. However, due to the patient’s MI 10 hours after the third revision and IV prostaglandin administration, the flap became pale and no further revision was carried out. Despite multiple revisions and good flow after each anastomosis intraoperatively, actual blood supply to the flap was most likely provided by collateral blood flow of the lower limb, which is suboptimal.
It is worth acknowledging that this incident of compromised flap signal happened just few hours after nitrates were administered to our patient. Our patient had received nitrates due to his hypertensive crisis. The association of intraoperative use of nitrates in a flap surgery as one of the factors associated with flap failure has remained controversial (Suominen and Asko‐Seljavaara, 1995; Simpson et al, 1996). In a hypertensive crisis, systemic nitrate administration decreases systemic vascular resistance to reduce arterial blood pressure. As combination of perfusion pressure changes and small cross-sectional area of blood vessel, it influences the blood flow to the flap negatively. The systemic vasodilation may cause shifting of blood flow from an already maximally vasodilated free flap (Banic et al, 1999) and may cause reflex vasoconstriction of the flap when nitrates administration stops (Adams and Charlton, 2003), leading to arterial thrombosis and contributing to its failure. Such incidents can be also viewed similar to a steal syndrome.
Steal syndrome causing flap necrosis has been sparsely reported in literature and remained hypothetical (Young et al., 2018) as compared to the more commonly reported cases of steal syndrome causing partial limb loss after a free flap reconstruction (Murphy et al, 2021). Alternative drugs that may be considered instead of nitroglycerin include slow IV labetolol and nicardipine, which is commonly used with cases of hypertensive crisis accompanied with target organ damage, such as in accompanying acute renal failure (Marik and Rivera, 2011).
Fluid maintenance is vital to maintain blood flow to free flap and is one of the predictors of flap failure. It can achieved via hyperdynamic fluid resuscitation using a combination of colloid and crystalloid, but not exceeding 6 ml/kg/hour as it may lead to oedema. This can be guided by ensuring urine output to be equal or more than 1 ml/kg/hour, normal blood pressure, while maintaining haematocrit between 30–40% (Brinkman et al, 2013). Our patient had sufficient fluid resuscitation.
Prostaglandin was used in our patient during his hypertensive crisis. It is described in the literature as an effective vasodilator; however, there is little information regarding its effect on acute MI, but it has been shown to be a protective cardiovascular agent (Zhu et al, 2017).
However, even with the most careful and meticulous technique, other factors still need to be considered in determining a flap success. Perhaps, a conventional angiography would be beneficial in preoperative assessment of dynamic lower limb distal circulation, which are the three main arteries of the lower leg (posterior tibial, anterior tibial and peroneal arteries). A CT angiography could also have been done to assess any distal interruptions of the lower limb arteries. Additionally, an echo or elastography could have been performed to assess arterial wall thickening due to arteriosclerosis. We learned that when retrograde perfusion is sufficient a Doppler signal can be heard in an old occluded vessel.
Increased operation time of >10 hours has been described as a strong predictive factor in flap necrosis (Pattani et al, 2010). In our case, total operation was 9 hours due to difficult anastomosis and problematic vessel. Age has been described as an insignificant predictive factor for flap necrosis, but in cases with several confounding comorbidities, such as the underlying ischaemic heart disease in our 80-year-old patient, it is likely to represent a more significant factor (Pattani et al, 2010). One study has shown that patients ≥90 years are able to benefit from free flap reconstruction with favourable long-term outcomes (Wester et al, 2013).
Conclusion
Vascularised lymph node transfer in lymphoedema patients has shown high success rate with low rates of complication and failure (Mardonado et al, 2017). SCIP flap were chosen in our case as it has fairly easy access to the donor vessel, is highly vascular and has low donor site morbidity.
We propose that systemic administration of nitrates has triggered the catastrophic event, aggravated further by the pre-existing poor arterial vessel morphology and an old total occlusion of tibial posterior artery, which was detected not before the third revision.
Systemic vasodilators should be avoided for our future cases as we believe it can cause steal syndrome in a free flap. Preoperative Doppler signal may not be sufficient in multimorbid patients in preparation for free flap surgery. Due to false positive Doppler signal of distal pulses, angiography should be performed to maximise the safety of multimorbid patient and success rate of a free tissue transplantation.
In all cases of major free tissue transplantation, a thorough history especially in elderly patients, needs to be collected. Should there be any evidence of high risk, a decision not to perform free tissue transplantation would be the best option.