The World Health Organization (WHO, 2023) defines eHealth as: “The cost-effective and secure use of information and communications technologies in support of health and health-related fields, including health-care services, health surveillance, health literature, and health education, knowledge and research.” eHealth encompasses a wide range of modalities that utilise digital technology, including robotics, artificial intelligence, wearable devices connected to smart phones, electronic health records and databases, telehealth and virtual consultations via video, mobile health (mHealth) including apps, and online information systems such as websites and online courses (Oh et al, 2005; Borrelli and Ritterband, 2015; Chan, 2021).
A patient-centred health system is one that prioritises the needs of patients (Robinson et al, 2008). Virtual consultations via telehealth, for example, are one way of creating a more patient-centred health system by making care more convenient to patients (McGrail et al, 2017; Tebeje and Klein, 2020). With the increasing adoption of eHealth technologies, patients may benefit from a more personalised and integrated approach to lymphoedema care.
Exploring a classification system for the different types of eHealth
A model for understanding how to classify eHealth modalities has been developed by the WHO (2018). The WHO classified digital health interventions by the ways digital and mobile technologies are being used to support health system needs. In this model, digital health interventions are organised into four groupings based on the targeted primary user (Table 1).
Under each category are subcategories of interventions and examples of various types of technology that can be used to achieve the overarching group function.
One example of interventions for clients (Figure 1) is “targeted client communication”. Hawkins et al (2008) state that this allows for separate audience segments (often demographic categories) to benefit from a shared message. Targeted client communication can be achieved in several ways, including sending health event alerts to specific population groups, health information based on health status or demographics, targeted alerts and reminders, and diagnostic results. Health promotion through mHealth and mobile phone SMS alerts is one way in which targeted health communication can be delivered.
Despite the fact that research in eHealth for lymphoedema care is in its infancy, Mangion et al. (2023) have demonstrated the existence of a wide variety of use cases. The WHO model is applicable to lymphoedema as demonstrated with intervention examples (Table 2).
The rationale for using eHealth
Healthcare may become more accessible, efficient and effective by leveraging digital technologies to improve accuracy of care, access to care, and decrease treatment costs. It may also facilitate communication, patient engagement and information sharing for enhanced condition monitoring and symptom management.
Enhancing accuracy of care
eHealth has the potential to improve the accuracy of lymphoedema care in several ways. For example, robotic-assisted surgery is being used to reduce surgeon error and improve outcomes in lymphadenectomies and lymphaticovenous anastomosis procedures (Maeso et al, 2010; Gkegkes et al, 2019; Chen et al, 2021; Lindenblatt et al, 2022).
The potential benefits of robotic-assisted surgery include improved precision, increased dexterity during surgery, better lymph node retrieval timing and decreased incision size (Moorthy et al, 2004, Lee et al, 2017, Ahn et al, 2023). In the case of lymphadenectomies, robotic-assisted surgery may have the potential to reduce the risk of complications such as postoperative lymphoedema.
In a systematic review by Gkegkes et al (2019), only 4 out of 51 patients (7.8% over a variable follow-up period from 2 to 67 months) reported lymphoedema following robotic-assisted lymphadenectomy. Within the group the number of dissected lymph nodes ranged between 5 and 34. This rate of post-operative lymphoedema is lower than has been reported for traditional surgery types (Chen et al, 2022b). This is particularly important, given that morbidity is higher for inguinal lymphadenectomy compared to cervical or axillary lymphadenectomy, as found in a review by Sarnaik et al (2009).
Additionally, patient satisfaction rates have been reported to be higher in robot-assisted surgery procedures compared to conventional surgery (Chen et al, 2022a). One reason for improved satisfaction, as described by the authors, could be that the robot technology can assist with aesthetically pleasing incisions, which the authors describe being: “Typically due to less traumatization and lack of hematoma-related complications.”
eHealth technologies are being used to diagnose lymphoedema remotely and improve the accuracy of monitoring and treatment. For example, remote surveys and telemedicine consultations have been shown to help healthcare practitioners identify lymphoedema symptoms earlier and make more informed decisions about treatment (Fu et al, 2018; Gabe-Walters and Noble-Jones, 2021; Noble-Jones et al, 2021).
Furthermore, 3D scanning and imaging devices are being developed to accurately measure limb volume and track changes in the affected limb over time, which may be especially useful in monitoring the progression of lymphoedema (Lu et al, 2013; Ohberg et al, 2014; Yaghoobi Notash et al, 2022).
Improving access to care and reducing treatment costs
Technologies such as telehealth and remote monitoring allow lymphoedema patients to receive care from their own homes, which is important for patients who live in remote or rural areas (Moffatt and Eley, 2010). This can improve access to care and reduce the need for patients to travel long distances to see their healthcare practitioners.
This may also lead to reduced costs. Naumann et al (2023) compared 55 individuals who received telehealth and in-person care following breast cancer surgery. They found that the median attendance costs per participant was AU$39.68 (range $28.52–$68.64) for telehealth and $154.26 (range $81.89–$251.48) for the in-person cohort, an average cost saving of $114.58 per session.
Improving communication and enhancing patient engagement
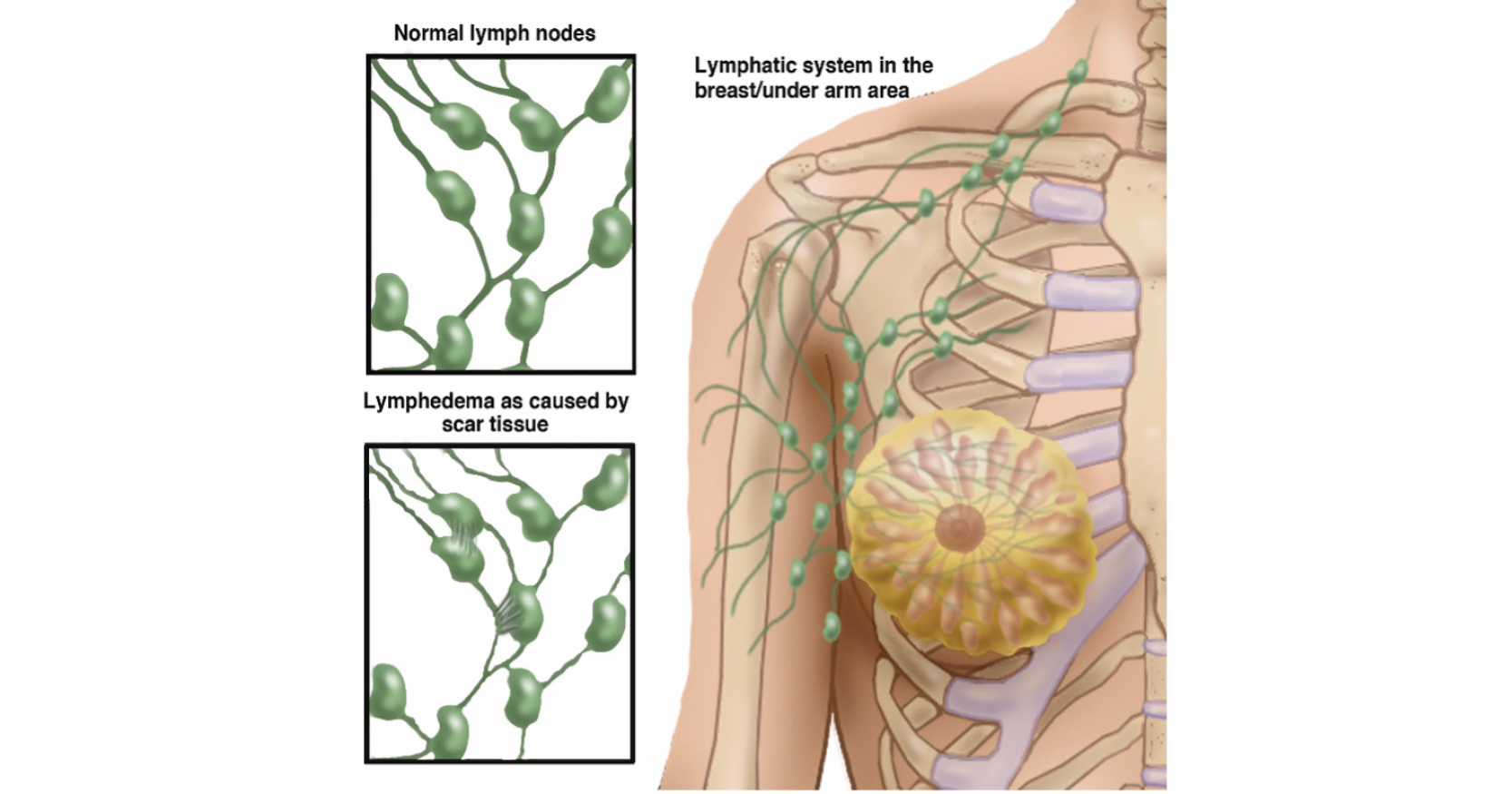
Using eHealth tools may help lymphoedema patients learn remotely and be empowered in their self-care. Complex concepts, such as how the lymphatic system works and how to perform exercises, can be explained through video technology and online avatars, which improves communication and, therefore, patients’ ability to engage with lymphoedema concepts.
Further research is required in this area, but an example of research investigating eHealth was a study by Fu et al (2022). They reported on a randomised controlled trial of a web and mobile app with a programme of exercises designed for breast cancer patients to manage chronic pain and lymphoedema symptoms, providing them with more information about their condition and empowering them to make informed decisions about their care. At the 12-week endpoint, the authors found that the patients using the app had significant improvements in chronic pain, arm and hand swelling and heaviness. Usability and feasibility testing demonstrated that “Patients love the web-based program, especially the videos using the avatar technology to demonstrate the complicated lymphatic system, and illustrate the physiological functions of each exercise and detailed step-by-step instructions for each exercise.”
Enhancing information sharing for improved condition tracking and symptom management
eHealth solutions may help healthcare practitioners monitor lymphoedema patients more closely and adjust treatment plans as needed. For example, Kalinga et al (2022) reported on mobile phone-based text messages being used to assist community health workers with reporting of cases of lymphatic filariasis morbidity in Tanzania. Not only did the eHealth technology help to improve patient reporting, but it also assisted with simplifying the exchange of information between lower and higher levels of management within the health programme.
Improving outcomes of complex lymphatic therapy
Complex physical therapy (CPT) is a comprehensive treatment approach used to manage lymphoedema, which can involve a combination of lymphatic drainage, compression therapy, exercise, and skin care (Casley-Smith and Casley-Smith 1992). eHealth technologies have the potential to improve outcomes of CPT. For example, Pawar et al (2022) reported on a prototype robot that has been developed to improve lymphatic drainage. The prototype lymphatic drainage robot is programmed to stimulate the lymphatic system. The robot climbs up the limb, applying radial pressure on the skin to remove the excess fluid into the lymph vessels towards the upper side of the limb.
Further research and industry opportunities
There are many research and industry opportunities related to eHealth and lymphoedema care that involve examining the efficacy and feasibility of interventions as well as governance, legal and ethical concerns.
Efficacy and feasibility
There is the need for rigorous research to evaluate the effectiveness of eHealth technologies in lymphoedema care. eHealth resources need to be designed appropriately with consideration of factors such as efficacy and impact on patients lives, as well as feasibility, accuracy and factors such as complexity which impact usability.
For example, one study looking at online resources for lymphoedema found that resources were above the recommended levels for readability and complexity, which has consequences for people living with lymphoedema (Tran et al, 2017). The authors stated: “The suitability level is barely adequate for the intended audience.” Therefore, eHealth resources need to be designed keeping the end user in mind.
Another consideration is the assessment of the quality of eHealth resources placed for free for public access on the internet, such as via the social media platform YouTube. A study of 90 free educational videos about lymphoedema rehabilitation on YouTube found many were of poor quality, with the authors concluding: “The biggest obstacle for YouTube to be an excellent source of information is that it hosts large volumes of uncontrolled and low-quality data” (Küçükakkaş and İnce, 2022). The authors also state: “Videos uploaded under the headings of like sexuality, violence, racism, and copyrights are subject to a specific checking process. However, this type of control is not in question especially in medical videos.” It is, therefore, important that health practitioners assess the quality of free online content before encouraging patients to search online for information.
Governance, legal and ethical concerns
eHealth poses important ethical, legal, and regulatory challenges related to data privacy, security, and equity, which need to be addressed to fully realise its potential benefits. For example, informed consent on an app requires a balance between convenience and appropriate disclosure. Zegers et al (2021) discuss the fact that consent on commercial mobile apps typically consists of checking a box and that users rarely read the terms and conditions.
If eHealth is to revolutionise healthcare systems, there must be governance systems in place to help healthcare systems adapt. The National eHealth Strategy Toolkit is designed to guide policy-makers and was developed by the WHO and International Telecommunication Union (2012). It is a resource for establishing national eHealth/digital health strategies, which are necessary for national governance and a supportive ecosystem for digital health.
Conclusion
eHealth represents a rapidly growing field that is transforming the way healthcare is delivered and experienced. Ongoing research on eHealth in lymphoedema, industry support, and policy leadership are required.