The enhanced recovery after surgery (ERAS) protocol is a standardised set of evidence-based, multimodal interventions and principles, designed to reduce the physiological stress of surgery and facilitate return to pre-operative levels of organ function. First described by Henrik Kehlet in 1997 in relation to colorectal surgery and initially named the “fast-track surgery” pathway (Kehlet, 1997), ERAS protocols are now in use across a number of surgical specialties.
ERAS protocols are multidisciplinary and encompass pre-operative (e.g. nutrition optimisation), intra-operative (e.g. use of short-acting anaesthetic agents) and post-operative (e.g. early mobilisation) interventions. Use of an ERAS protocol has been shown to reduce healthcare costs, without compromising clinical outcomes (Paton et al, 2018). One comparison of 50 patients undergoing colorectal surgery using an ERAS protocol, with 50 patients treated before the protocol’s implementation, found a shorter average length of stay in the ERAS group (7 days vs 10), as well as a lower rate of severe complications (12% vs 20%) (Roulin et al, 2013).
Shorter length of stay is associated with reduced morbidity, mortality and readmission, as well as benefits in healthcare resource utilisation. But as length of stay decreases, the importance of post-discharge surveillance for surgical wound complications (SWC) correspondingly increases, as such complications are increasingly detected in the community (Leaper et al, 2004).
Post-discharge surgical site infections
Surgical site infections (SSIs) occur in an estimated 0.5–3% of patients undergoing surgery (Seidelman et al, 2023), and can result in readmission to hospital, increased healthcare costs, slower wound healing and increased morbidity and mortality.
However, this is likely to be an underestimation of the actual rate (WUWHS, 2018). A systematic literature review found that 60.1% of SSIs became apparent only after hospital discharge (Woelber et al, 2016). In a Welsh study of 545 patients undergoing elective or emergency surgery, 13% developed an SSI within 30 days of surgery, with two distinct peaks of diagnosis: one at days 5–7, and a later peak at days 22–28 (Reeves et al, 2021). Time elapsed between surgery and clinically apparent infection also varies according to the type of surgery performed; for example, Staphylococcus aureus infection is diagnosed on average 14 days after plastic surgery, 24 days after general orthopaedic surgery, and 28 days after orthopaedic surgery including prosthesis implantation (Seidelman et al, 2023).
SSI surveillance — active and prospective monitoring and reporting of SSIs — was the subject of a recent best practice statement (Wounds International, 2023). The statement made a range of recommendations on implementing surveillance programmes within routine clinical practice, and how the data could be used to ensure delivery of high-quality patient care. Current best practice standards recommend following up patients undergoing surgery for 30 days after hospital discharge, to assess the development of any infection – although as indicated by the average time to diagnosis of S aureus infection, for some surgeries an even longer follow-up period may be prudent. In practice, hospitals are not always equipped for this level of post-discharge surveillance (Woelber et al, 2016). In the Welsh study, almost half (49.3%) of the infections were diagnosed by primary care, and more than one-quarter (28.2%) were managed entirely in community care (Reeves et al, 2021).
Early detection of SSIs is important to enable timely intervention and reduce the risk of more complex complications developing (Sandy-Hodgetts et al, 2020). At the population level, SSI surveillance drives improvement in clinical practice, assures patient safety, tracks changes in infection rates, and provides patients with accurate information to make informed decisions (Wounds International, 2023). Post-surgical care must therefore include informing and engaging patients in their care (Sandy-Hodgetts et al, 2020), as well as identifying the presence of factors that are known to increase the risk of SWC development [Table 1].
The role of wound dressings in supporting surgical wound healing
Dressing selection is an important part of post-operative care; appropriate dressing choice can positively impact clinical outcomes by protecting the wound during healing and reducing the risk of infection (Morgan-Jones et al, 2022). An expert global consensus identified six characteristics of post-surgical dressings that were considered key requirements for use in managing surgical incisions (Morgan-Jones et al, 2019):
- Flexibility and elasticity (to avoid impeding movement or pulling on the skin);
- Good fixation to the skin on application;
- Absorbency and ability to handle exudate;
- Skin protection (avoiding excessive adhesion, blistering or irritation);
- Water-resistance, providing a good seal/barrier function and enabling the patient to shower;
- Minimisation of dead space where necessary where fluid can pool.
Undisturbed wound healing is a topic that has gained traction in recent years (Morgan-Jones et al, 2022). In the absence of factors such as suspected infection or excessive bleeding that necessitate a dressing change, leaving dressings in place for longer periods offers benefits such as optimised healing, reduced risk of contamination, and savings in cost and clinician time (Brindle and Farmer, 2019).
Transparent dressings may be considered advantageous in such circumstances, by allowing increased surveillance without the need to remove the dressing (Sandy-Hodgetts et al, 2020). When used appropriately, these dressings can support patient engagement by involving them actively in post-discharge surveillance and care. The ISWCAP best practice statement in 2020, aimed at improving identification and prevention of SWC, recommended that “novel strategies for patient engagement should be used to aid early identification of SWC wherever necessary (e.g. dressings that allow visibility without removal, telemedicine in rural areas, new diagnostic technology, smart phone applications, validated fit-for-purpose risk assessment tools”; Sandy-Hodgetts et al, 2020). In a survey of staff in adult cardiac surgery centres, most respondents already used digital systems, including photo sharing, for post-discharge remote wound monitoring (Tanner et al, 2023). These systems can reduce staff workload burden, speed up data collection, and improve access to care for patients. Rochon et al (2021) conducted a study in two cardiothoracic centres using a digital post-operative surveillance platform, where patients were periodically asked to upload photographs of their wound. The platform was well received, with 87.3% (138/158 patients) submitting at least one photograph.
Digital systems could be combined with the use of other novel strategies such as transparent dressings, as in a study currently underway to evaluate the use of a transparent hydropolymer dressing in conjunction with smartphone technology, to facilitate remote wound assessment without the need for patients to visit a clinician in person (Sandy-Hodgetts et al, 2022).
Leukomed® Control transparent dressings
Leukomed® Control is a sterile, transparent, absorbent island dressing, comprising a semi-permeable polyurethane film and a hydropolymer wound pad. The absorbent hydropolymer pad absorbs exudate while maintaining partial hydration, and the permeability of the polyurethane film to water vapour and air prevents the build-up of fluid that could lead to maceration and infection. Leukomed Control dressings are suitable for use on dry or low exuding acute wounds, including surgical wounds.
As a transparent dressing, Leukomed Control offers opportunities to monitor wound healing without the need to remove the dressing. The dressings have a wear time of up to 14 days.
Clinical evaluation
The clinical evaluation assessed patients from the Torrecárdenas University Hospital (Almería, Spain) who underwent cholecystectomy between January 2020 and June 2023. This was a single-arm observational study. The study enrolled adult patients of both genders, aged 18 years and older, who were undergoing open or laparoscopic cholecystectomy at the hospital and had agreed to take part in the research.
Data was collected through a review of the patient’s medical records, with the primary focus on assessing the successful healing of the surgical wound. The secondary variables encompassed patient background information (such as gender, age, height, and weight) as well as the identification of any concurrent comorbid conditions. Surgical wounds were assessed for the presence of exudate or signs of infection at baseline (first application of a Leukomed Control dressing on the day of surgery) and again at the final visit. Evaluation data was also collected in a variety of categories related to the performance of the dressing, and patient and HCP satisfaction with the dressing choice. [Box 1]
Baseline characteristics
A total of 101 patients were included in the evaluation. The average age of participants was 55.5 years (range: 28–89 years), and 69 (69%) were female.
The average body mass index (BMI) of participants was 26 kg/m2 (range: 20–35 kg/m2). 15 people (15%) had a BMI of 30 or above, corresponding to a diagnosis of obesity as defined by the World Health Organization (WHO Fact Sheet).
Over half – 53 (53%) – had a concomitant condition recorded. The conditions recorded were circulatory disorders (22 patients), hypertension (15 patients), diabetes (14 patients) and obesity (2 patients) – although as noted above, a further 13 patients had a BMI corresponding to a definition of obesity but did not have a diagnosis of obesity recorded in this evaluation.
All patients underwent cholecystectomy: 24 patients underwent open cholecystectomy (2 of them with Kehr’s type [T-tube] drainage), and 77 underwent laparoscopic cholecystectomy. None of the patients had signs of infection at their initial visit, although two patients did have bloody exudate from their wounds.
Results
The average time elapsed between day of surgery and the final follow-up visit was 8.06 days (range: 7–10 days) [Figure 1].
Patients undergoing open surgery had 1 dressing applied after surgery; those undergoing laparoscopic surgery had 3 or 4 dressings applied (one for each surgical wound). The average time elapsed between the first and last visits was similar between the surgery types: 8.25 days for open surgery, and 8.00 days for laparoscopic.
The two patients with wound exudate at baseline continued to have low output of bloody exudate at their final visit. No other patients developed exudate over the course of follow-up, and none of the 101 patients had any signs of infection at their final visit.
All participants reported “very good” dressing retention and “very good” exudate control. The adhesion of the dressing was good in all cases, with all 101 patients reporting “strong” adhesion and “strong” adaptation to the wound bed. Dressing removal and dressing handling were both rated as “easy” in every patient, and the ease of application was rated as “excellent” by every patient as well as by the treating clinician.
Patients were asked to rate their comfort level; all patients rated the dressings as “very comfortable”, indicating that they were hardly aware of the dressing while it was being worn. All replied that they experienced no pain associated with the dressing. Every patient reported that they were satisfied with the Leukomed Control dressing, and that they would positively recommend its use.
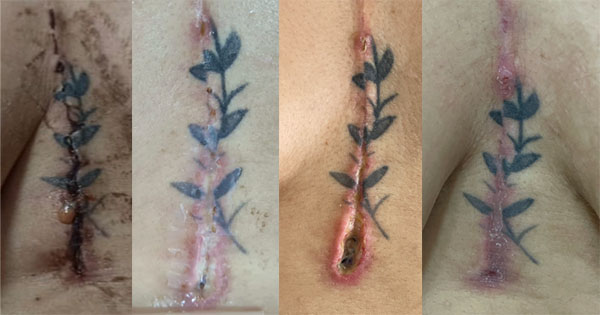
Almost all wounds – 99 (99%) – had healed by the end of the follow-up. Two patients had wounds that were considered to have improved, but had not healed; however, their treatment objectives were considered to have been achieved. No adverse events were reported in any patients. Box 2 reports on two cases from this evaluation.
Discussion
SSIs pose a significant challenge in healthcare, leading to increased morbidity, prolonged hospital stays, elevated costs, and an adverse impact on the patient’s post-operative recovery experience. It is reported that up to 25% of patients undergoing colorectal surgical procedures develop an SSI (Reeves et al, 2021), necessitating vigilance in post-operative care. ERAS protocols have been instrumental in improving surgical outcomes and early discharge from hospitals, effectively reducing complications overall. However, the earlier discharge of patients under ERAS has a potential drawback – up to 50% of SSIs develop in the community, and this may lead to underestimations of the true SSI rate due to inadequate follow-up beyond 30 days after hospital discharge (Reeves et al, 2021). This shift in post-surgical care provision provides an opportunity to review and “modernise” prior SSI surveillance methods (Tanner et al, 2023).
The study by Reeves et al (2021) highlights the limitations of the ERAS protocol in identifying SSIs that develop in the community setting, which can lead to inaccurate SSI data. This issue emphasises the need for innovative solutions to bridge the gap between hospital care and community follow-up. One such potential solution is the use of advanced transparent dressings like Leukomed Control, which can be left on the patient for up to 14 days without removal. These dressings offer a unique advantage in terms of continuous monitoring, improving detection of SSIs and other complications in the community.
Transparent dressings allow for ongoing patient education and self-monitoring of surgical wound sites. Patients can be empowered to watch for early signs of infection or complications, potentially leading to quicker intervention and improved outcomes.
In practice, patient attitudes towards wound visibility may vary, with some preferring to have increased visibility for better engagement in their care, which can have a positive impact on wound healing, treatment, and overall well-being. Maintaining undisturbed wound healing is encouraged, and transparent dressings offer a clear advantage in visualising the wound site without the need for removal, reducing the need for unnecessary dressing changes and thereby minimising disruption to the wound bed and surrounding skin.
In the current evaluation, Leukomed Control dressings were well-tolerated and effective in promoting wound healing in all cases. All but two patients had complete wound healing within 10 days of surgery; both of the patients whose wounds had improved but not healed had pre-existing circulatory disorders, which may have contributed to their incomplete healing.
The dressings demonstrated many of the features of an “ideal” post-surgical wound dressing, including good adhesion, skin tolerability and absorbency. Importantly, they were viewed favourably by patients, who reported finding them comfortable during wear time of up to 10 days.
The patients enrolled in this evaluation including a number with risk factors that may predispose them to development of infection, including 15% with obesity, 22% with circulatory disorders and 14% with diabetes. Despite this, none of the patients developed any signs of infection during the follow-up period.
The existing shortcomings in current standard of care and practice in the detection and prevention of surgical wound complications such as SSIs highlight the promise of advanced transparent dressings such as Leukomed Control. It offers continuous monitoring, early detection, and patient engagement, potentially improving outcomes, reducing healthcare costs, and ensuring more accurate SSI data.
Conclusions
Use of an ERAS protocol can reduce length of stay after surgery and support earlier discharge; however, as most SSIs become apparent after discharge, strategies are needed to support the earlier identification of complications and enable timely intervention. Leukomed Control dressings are well-tolerated and effective in managing surgical wounds, and with their flexibility and transparent nature, may support the transition from hospital to community care by allowing patients and primary care clinicians to more easily monitor for early signs of infection.